Preggie Pals
Foetal Non-Stress Tests During Pregnancy
[00:00:00]
Please be advised, this transcription was performed from a company independent of New Mommy Media, LLC. As such, translation was required which may alter the accuracy of the transcription.
[Theme Music]
DOCTOR JAN PENVOSE-YI: You may have heard of fetal non-stress tests but what is it? How are they performed? And under what circumstances are they recommended? I’m Doctor Jan Penvose-Yi, and today we’re discussing fetal non-stress test in pregnancy. This is Preggie Pals.
[Theme Music/Intro]
STEPHANIE GLOVER: Welcome to Preggie Pals, broadcasting from the birth education center of San Diego. Preggie Pals is you’re online on the go support group for expecting parents and those hoping to become pregnant. I’m your host Stephanie Glover. Thanks to all of our loyal listeners who’ve joined the Preggie Pals club. Our members get special episodes and bonus content after each new show plus special giveaways and discounts. See our website for more information. Another way for you to stay connected is by downloading our free Preggie Pals app, available in the Android, iTunes and Windows marketplace. Sunny, our producer is now going to give us some information about the virtual panelist program
SUNNY GAULT: Sure. Okay. So, if you aren’t here in studio with us but you still ike to participate in the conversation, there’s a couple of different ways you can do it. You can like our Preggie Pals Facebook page, you can also follow us on Twitter. And we’re going to be posting some questions that we’re asking our panelist here in studio and just sharing some information about non-stress test and what we’re learning today. It’s a great way if you want to ask our expert some questions. So, I’ll go ahead and post some stuff out there and feel free to comment as we go along
STEPHANIE GLOVER: Thank you. So we’re going to go around the table and introduce the panelists, so go ahead Amy?
AMY DUGAN: Hi my name is Amy Dugan. I am thirty-three years old. I am currently a homeschooling stay-at-home mom. So that is my occupation and I have two little girls. One and a half and five and a half and I have them both vaginally, praise the Lord because I do not want to deal with the c-section, so that was good
KIRSTEN STRATON: Hi I’m Kristen Straton, I’m a birth and postpartum doula and proud mom of three, ages five, three and one and I did have C-sections with my lovelies. And I’m here to talk about my experience with non-stress tests
STEPHANIE GLOVER: Great. Thank you
SUNNY GAULT: And you guys heard from me, but I’m Sunny, I’m producing today’s show. I’m also the owner of new mommy media which produces Preggie Pals as well as Twin Talks, The Boob Group and I’m missing one, Parent Savers. Okay. And I have four kids of my own. My oldest is four and I’ve got a two-year-old and then twins who will turn one year next week
STEPHANIE GLOVER: Great. Thank you. And I’m Stephanie, I’m the host of Preggie Pals. I’m thirty-two. I’ve got two little girls, three and fifteen months. My first was born C-section. My second VBAC and I don’t have personal experience with the non-stress test so I’m really excited to learn more.
[Theme Music]
SUNNY GAULT: Okay so before we start today’s show we have an interesting pregnancy headline that we thought we would share with you guys. And this headline says: baby Successfully Born via Womb Transplant. Will more follow? And the idea is, is that there is a mother who at fifteen found out she did not have a womb, and she enrolled in a trial, and basically received a uterus that have been donated by sixty-one-year-old woman. That transplant was a success. And she has welcomed, it says they welcome their first child. So, the baby’s been born, everything’s you know, everything seems to be going really well and they’re kind of touting this as an option for women with infertility issues. So wanted to kind of throw this out to you ladies to see what do you think about this? Is this kind of an unbelievable thing? Have you heard about it? Did you guys hear about this article before? Any ideas?
STEPHANIE GLOVER: I think it’s amazing. Goes to show the advances of science and really how they can affect families. Kristen you had a good point that I don’t think the article touched on is
KIRSTEN STRATON: Oh I was curious as to how much of her reproductive organ she was born with? Whether or not she had an egg donor as well if she had her own fallopian tubes and ovaries, or that was also something that she received from a donor?
STEPHANIE GLOVER: Right and I think I did see this article and I was trying to find it on my phone as well because I think there was one. I do think that the baby was born via C-section and I want to say maybe around thirty-six weeks. Now that I’m jogging my memory, but I don’t know the actual details of the labor, but, fascinating.
KIRSTEN STRATON: Yeah. If she had a transplant she would need a C, cesarean section just because of risk of rupture of [inaudible]
STEPHANIE GLOVER: Oh interesting
KIRSTEN STRATON: Yeah
SUNNY GAULT: It’s amazing kind of what they can do now with all of this. I know, my husband and I originally struggled. We had some infertility problems in the beginning. And they did all the tests and everything and found that it was probably just the timing issue with us because they couldn’t find anything wrong with us. But, I remember going through that whole process of thinking, well, what if we can’t have our own or you know how far would I go? And to know, you know there are a lot of couples out there that are struggling with infertility and maybe this is, you know, show some signs of being an option.
STEPHANIE GLOVER: Definitely
SUNNY GAULT: So, that’s nice
[Theme Music]
STEPHANIE GLOVER: Today we’re learning all about the fetal non-stress tests in pregnancy. Joining us here in the studio today is Doctor Jan Penvose-Yi. A board-certified obstetrician affiliated with Tri-City Medical Centre. Doctor Penvose-Yi has been practicing medicine for eight years and has delivered over six hundred babies. Welcome to Preggie Pals, thank you so much for joining us
DOCTOR JAN PENVOSE-YI: Well thanks very much for having me here today
STEPHANIE GLOVER: And so before we get started, tell us a little bit about your family. Are you a mother?
DOCTOR JAN PENVOSE-YI: I am, I’m also a mother. I’m a mother of three. My oldest daughter is fifteen and then I have a ten-year-old daughter and a six-year-old wild child son. I was lucky to get just before my menopause started to happen so
STEPHANIE GLOVER: Well, awesome. So you can comment then as a mom and as a doctor, that’s perfect
DOCTOR JAN PENVOSE-YI: Absolutely! Absolutely! Definitely, deliveries are interesting for each, each child you have
STEPHANIE GLOVER: They can certainly differ . . .
DOCTOR JAN PENVOSE-YI: Yeah
STEPHANIE GLOVER: Now, Doctor Penvose-Yi, what is a fetal non-stress test?
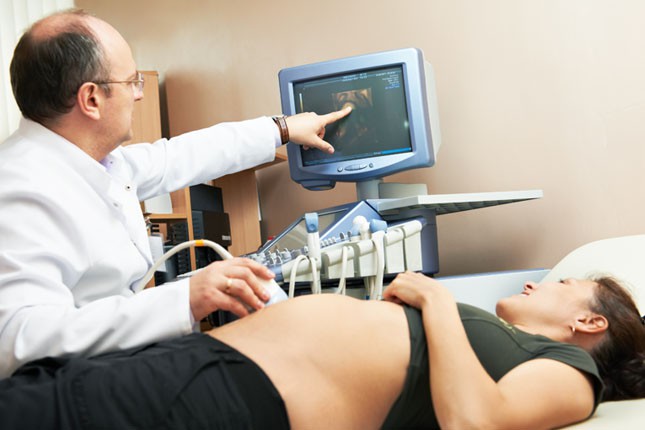
DOCTOR JAN PENVOSE-YI: So, a fetal non-stress test is a way of evaluating the well-being of a baby in utero. And it can be done before the baby’s delivered during the delivery process. I think today we’re focusing more on before the baby is delivered. Basically, we, you now all mom know about those monitors we put on your belly, but it’s a monitor that sends sound waves to the baby's heart to see the actual heartbeat of the baby. It’s a way to transcribe that onto a piece of paper and look for things about the baby’s heart rate and heartbeat that are reassuring or non-reassuring.
STEPHANIE GLOVER: Okay. And so, what does non-stress within like the title of the test indicate?
DOCTOR JAN PENVOSE-YI: So, originally one way we would test babies was actually a contraction stress test. And we wanted, and you’d have to induce contractions to see how the babies handle contraction and a mom that may or may not need to be delivered.
So, you wanted to do something less invasive and get similar or equal you know type results. So we found a way of just monitoring the heartbeat and then there are guidelines for what that means when the babies not stressed
STEPHANIE GLOVER: Interesting. When do they, stop doing the stress test? Because I do actually remember hearing about the stress tests and then all of a sudden I remember hearing about the non-stress tests and not really understanding the difference.
DOCTOR JAN PENVOSE-YI: I honestly don’t know or hear of that but I can tell you for as long as I’ve been in practice, I’ve never seen that contraction test used. However, it’s definitely an over-test and it’s a known way to evaluate a baby. But we don’t actually go over the way and do it.
STEPHANIE GLOVER: Yeah. Would it be like inducing labor essentially or?
DOCTOR JAN PENVOSE-YI: Well no it’s inducing contractions. Sometimes people get that confused and actual like contractions don’t always lead to labor.
STEPHANIE GLOVER: Right
DOCTOR JAN PENVOSE-YI: So, you would induce contractions. Of course, if there is something going on, sometimes the body might kick in labour because that’s sometimes a response of dealing with issues
SUNNY GAULT: So, you know when I have been in labor, they kind of do the same stuff where they hook up kind of the belts too and you monitor that, so would that be considered a stress test. I mean it may be natural that your body is contracting but would that be an example of the stress test?
DOCTOR JAN PENVOSE-YI: Like a contraction.
SUNNY GAULT: Yeah if you’re naturally having them.
DOCTOR JAN PENVOSE-YI: Yes. Well actually if you’re naturally having it, it is in some ways a contraction stress test.
SUNNY GAULT: Right.
DOCTOR JAN PENVOSE-YI: Absolutely.
SUNNY GAULT: okay.
DOCTOR JAN PENVOSE-YI: Absolutely
STEPHANIE GLOVER: So at what point in pregnancy are NST’s or you know non-stress test if I, if I use the abbreviation. At what point in pregnancy are they typically performed?
DOCTOR JAN PENVOSE-YI: So you can start performing them approximately twenty-six to twenty-eight weeks of pregnancy when the baby's neurologic development and physical cardiac development are advanced enough that you can interpret it .
STEPHANIE GLOVER: Okay so before it wouldn’t be as accurate then or
DOCTOR JAN PENVOSE-YI: Yeah it doesn’t mean the same thing before.
STEPHANIE GLOVER: Okay.
DOCTOR JAN PENVOSE-YI: Yeah.
STEPHANIE GLOVER: Now for panelists, did you guys have a non-stress test in your pregnancies?
AMY DUGAN: Yeah I did I had three, two with my first and then one with my second. My babies, they don’t want to leave so
SUNNY GAULT: They’re nice and warm, why would they leave?
STEPHANIE GLOVER: So did you have them later on in your pregnancy then?
AMY DUGAN: Yeah, for both of them. I had one on the due date for each of them and then with my first one, they said, oh your amniotic fluid is a little low. Go home, drink some water, relax, come in tomorrow, we’ll measure again. And everything was good, so we didn’t have to induce the next day. Luckily and I waited another week. I had them both at forty-one weeks.
STEPHANIE GLOVER: Okay
AMY DUGAN: So
STEPHANIE GLOVER: How about you Kristen?
KIRSTEN STRATON: Yes. I had them with my first multiple times. I had [inaudible 00:09:52] my entire pregnancy with my first two children
STEPHANIE GLOVER: And refresh us what does that mean?
KIRSTEN STRATON: It basically means that I could not stop vomiting. It’s just very, I guess the layman’s way to describe a very severe morning sickness but it’s really not morning sickness. So that involved a lot of IV hydration and a lot of trips to the ER. Sulfrin is another sort of anti-nausea medicine to help me carry to term. So a few times during my pregnancy I had preterm labor because I was so dehydrated and so that involved me seeing under observation at the hospital and getting the non-stress test done
STEPHANIE GLOVER: And how about how far along were you in that?
KIRSTEN STRATON: Definitely thirty weeks with my first and I think I had it again with my second at about thirty-six weeks because I, again had pre-term labor because of severe dehydration. And then with my third, I had them twice a week because I was very, very pregnant. I was almost ten months pregnant
SUNNY GAULT: Oh my goodness
KIRSTEN STRATON: So that was more just to make sure everyone was happy and healthy and there everyone was so
STEPHANIE GLOVER: And Sunny how about you?
SUNNY GAULT: Yes. So I had them a couple of times. I had them, my second child, I had gestational diabetes with him and so I can’t remember what week we started. I was trying to figure that out. But it was later in the pregnancy. And that was routine, you know, twice a week went in, Tuesdays, Thursdays. They’re very specific about what times you go and if I had to cancel it. Like, they needed to see me right away. I just remember being very specific, let’s put it that way. When I was pregnant with the twins they told me again it was going to have to be a routine thing. But, I ended up, you know, I went, I think I only had one appointment but it was supposed to be again like a Tuesday, Thursday or Monday, Wednesday thing. Something was supposed to be a routine. They started it at thirty-four weeks with me but I went into labour at thirty-five weeks so, yey I got out of it
STEPHANIE GLOVER: Well great and so I mean we can see the range of post-state or you know approaching due date, low amniotic fluid, pre-term labor, gestational diabetes, multiples, what are some other reasons for a non-stress test?
DOCTOR JAN PENVOSE-YI: One example would be like decrease fetal movement. If the mom just really not appreciate her typical pattern movement for the baby, that’s one reason. There are some maternal illnesses, something with chronic hypertension or autoimmune disorders. Those are other reasons we might do it. Somebody who has a history of fetal loss with their last pregnancy usually will initiate the testing. And you know, there may or may not be good studies on exactly when to initiate the testing but typically in my practice what we’ve done is a week or two before the loss or monthly, you know depending on how dramatic everything was. So at least, you know and if it is a term loss we’ll pick arbitrarily like thirty-six weeks or something to really you know pump up the monitoring including non-stress test and other forms of testing
STEPHANIE GLOVER: Right. And so if you’re kind of looking later on to if they have lost before then if you would need to deliver you’d have a better outcome by waiting kind of . . .
DOCTOR JAN PENVOSE-YI: Right. And plus, yeah, and plus you can, you know, just reassure the mom. So, sometimes it’s, it’s more for reassurance than to actually tell us exactly what’s going on but it’s a way that we as physicians and patients reassure ourselves
STEPHANIE GLOVER: Go into it with less fear or maybe less anxiety
DOCTOR JAN PENVOSE-YI: Right, right. Right, right
STEPHANIE GLOVER: Okay. And are there risks associated with this type of test to mom or baby?
DOCTOR JAN PENVOSE-YI: Not really. It’s basically sound waves that were reflecting off the baby’s heart. I know some people fear that their babies getting radiation from it, but it’s truly not radiation it’s not harmful it’s just sound waves
STEPHANIE GLOVER: Okay. And then how does the test actually detect the fetal distress or maybe other problems. So what are you looking for when you’re doing this test?
DOCTOR JAN PENVOSE-YI: So what you’re looking for is the variability of the heart rate. So we don’t want to see a straight line. We want to see little bumps and humps going up and down. And then we’re looking for large accelerations for a period of time. You know usually twice within the twenty to thirty-minute period that you have for guidelines. So you’re looking for accelerations of the fetal heart rate. You’re looking for a good beat to beat you know non–specifically variability. And you’re looking for not having decelerations
STEPHANIE GLOVER: Okay
DOCTOR JAN PENVOSE-YI: So if you have a deceleration that warrants for their testing
STEPHANIE GLOVER: Okay
DOCTOR JAN PENVOSE-YI: Yep
STEPHANIE GLOVER: And are you, I think I read there’s an association with watching kind of baby’s movements and how the heart rates to test those movements
DOCTOR JAN PENVOSE-YI: So that’s further testing via biophysical profile which the non-stress test can be part of
STEPHANIE GLOVER: Oh okay
DOCTOR JAN PENVOSE-YI: We can look at the fluid around the baby. We can look at the activity of the baby both finer movements and gross body movements. And we look for at certain gestational ages, we can look for practice breathing movements in a baby
STEPHANIE GLOVER: When we come back we’ll discuss more about fetal non-stress test including why are they performed , we’ll be right back
[Theme Music]
STEPHANIE GLOVER: Welcome back, today we’re discussing fetal non-stress test in pregnancy. Doctor Jan Penvose-Yi is our expert. Where are non-stress test performed? Are they in the OB office, in the hospital?
DOCTOR JAN PENVOSE-YI: Non-stress test can be performed in the office or the hospital
STEPHANIE GLOVER: Okay
DOCTOR JAN PENVOSE-YI: Or both. Sometimes we, you know, depending on the line of patients w have waiting for their non-stress test in the office, depending on the results we get we may then send them to the hospital for further non-stress testing. Some offices don’t have that facility, so they will just send their patients directly to the hospital. Or for people with twins like we talked about earlier or growth restrictions. They’re going to be on regular monitoring. They can either have that schedule at the office or the hospital. And sometimes are following with the high risk obese specialist. And they may do it there as well as your own office
STEPHANIE GLOVER: And who would perform it? Does the OB do it or a nurse or?
DOCTOR JAN PENVOSE-YI: So basically the nurses are trained to hook the patients up to the monitor, and they hook them up both to a contraction monitor and the fetal heart rate monitor. And then the physicians or the nurse practitioners or the nurse-midwives in the office can interpret the results and decide how to progress whether we want to further monitor or send out for more monitoring or do different monitoring
STEPHANIE GLOVER: Okay and so if a mama is told, okay you need to have a non-stress test, can you walk us through what she should expect from the time she gets in to the office or, or even if there’s anything she needs to know ahead of time to prepare
DOCTOR JAN PENVOSE-YI: Basically she should know that it’s just a means of evaluating the baby and it could be for a variety of reasons which we discussed earlier. And it’s nothing to worry about. And we tell her that we’re going to hook you up to these monitors and hopefully, we had better chairs, not too uncomfortable for because it’s a good twenty minutes. And the baby’s can be a little stinkers and hard to find especially the younger gestational ages. They’re kind of, they, I always say they can skit around more and have more room in there to hide from you. And if a woman’s got a little extra weight on her belly, that can make it harder to monitor the baby. So, you know, we have to tell people, you know, we’re trying to make you comfortable but we may have to shift the monitors. Sometimes the physician or midwife has to come in and help read to us the monitor. And it should be on the table trying to gear you in a comfortable position, you know, traditionally we like women to lay on their left side for best results. It keeps the blood flow best to the baby and the mom.
STEPHANIE GLOVER: Okay. So she will be laying down then to the
DOCTOR JAN PENVOSE-YI: She’ll be, usually in a recliner or lying on the bed that’s, you know, we don’t want to put moms flat
STEPHANIE GLOVER: Right
DOCTOR JAN PENVOSE-YI: So I think everybody kind of knows that we don’t just lay flat after twenty weeks of pregnancy. And that she’s just got to rest and usually she’s got all those kids running around with her oftentimes, I should say that. And so we, in my new office, I want to try to keep the kids happy and the moms happy and keep people comfortable
STEPHANIE GLOVER: Oh that’s so hard I remember of having to take my toddler
DOCTOR JAN PENVOSE-YI: Yes it is
SUNNY GAULT: Seriously
STEPHANIE GLOVER: Sit down
DOCTOR JAN PENVOSE-YI: Yeah
STEPHANIE GLOVER: Don’t touch that
DOCTOR JAN PENVOSE-YI: Yeah. And there’s various, you know, some people, one question is, oh should I have sugar to make my baby move more . . .
STEPHANIE GLOVER: Or do you need to drink more, eat more, anything like that . . .
DOCTOR JAN PENVOSE-YI: I mean certainly the babies have their normal sleep cycles and we may or we may not be able to wake them out of them truly. Usually, we’ll give our moms a cold glass of water if the baby’s seems to be sleeping and there’s no really good studies to show that the sugar or the cold glass of water. There is a, you can do an acoustic vibrations stim, stimulation to the baby, there’s machines for that. Honestly I sometimes tell the mom just poke that baby around, see if you know, see if it’s, if it’s asleep then you can wake it up, you know. But again there are not studies for that one. But it works, it works sometimes you just kind of choose them awake. And like you were saying about specific times for testings, I don’t give my patients a specific time but I usually do like to know, moms will know especially the ones that come regularly when their baby’s sleeping. So we try not to schedule when we know every time that baby’s going to be sleeping when they come so, for best results.
But yes so basically plan twenty-thirty minutes on a table maybe a little longer depending on how stinky the baby’s been that day. And then it may be followed up with something like an ultrasound to further evaluate like a biophysical profile
SUNNY GAULT: That was always part of the process for me. In fact, it always started with an ultrasound where they look at the amniotic fluid and it was specially, you know, when I had it with my twins, the couple of appointments that I did have, they were always looking at making sure everything was looking good and I wasn’t going in a preterm labor, all that good stuff. But yeah, that was always part of it. And they usually set me in a specific area for that and then I usually had to move to another bed where they actually hook up the, you know, straps and did that. And another thing I have to say is that ice helps a lot too. You mention the cold water, for some reason
STEPHANIE GLOVER: Externally you mean?
SUNNY GAULT: Yeah well not like for me then just like to wake up the baby. For some reason my medical care provider has the best ice. I know this sounds crazy but if I try to make that ice at home it wouldn’t work. So that was one of the nice things of going there is getting that ice and usually it did wake up the baby a little bit.
DOCTOR JAN PENVOSE-YI: It’s like that sonic crunchy ice . . .
SUNNY GAULT: It is
DOCTOR JAN PENVOSE-YI: Yes I’m pretty sure they just get a delivery from sonic and it is just ice for women who need to wake up their babies.
STEPHANIE GLOVER: And do women ever fall asleep during one?
DOCTOR JAN PENVOSE-YI: I f we get them comfortable enough to, maybe, yeah
STEPHANIE GLOVER: I feel like once you’re a mom like particularly if you could get in without your toddler I could fall asleep with the dentist. Anything just becomes a spot to experience
DOCTOR JAN PENVOSE-YI: If you’re on your own yeah
STEPHANIE GLOVER: Especially with ice
DOCTOR JAN PENVOSE-YI: Yeah
STEPHANIE GLOVER: Yeah with a good ice.
DOCTOR JAN PENVOSE-YI: A good book may be tell mom to bring a good book or . . .
STEPHANIE GLOVER: Or listen to a podcast. I don’t know I mean thirty minutes. So how are the test results reviewed with mom and when does she get those results
DOCTOR JAN PENVOSE-YI: So usually right at the time of the non-stress test because we’re going to tell her what the results are and should we do more or when we’re going to repeat it again. If we’re going to repeat it again
STEPHANIE GLOVER: Okay. So at least there’s not a long week
DOCTOR JAN PENVOSE-YI: Right, right, right and you don’t have to show them the strip or anything. You can say okay looks good, this is what we see or oh you know what sometimes, you know, this isn’t perfect so this is what we’re going to do
STEPHANIE GLOVER: Okay and if they were to need to comeback is it typically within just a few days or is it, does it really just depend on the situation
DOCTOR JAN PENVOSE-YI: if you’re doing prolonged monitoring, planned to monitor it can be anywhere from once a week to twice a week
STEPHANIE GLOVER: Okay
DOCTOR JAN PENVOSE-YI: Yeah. If it’s like, like come and see my baby’s like not moving like normally but the rest of the pregnancy has been uncomplicated if the strip looks good that day, then we’re not going to repeat it unless there’s an indication
STEPHANIE GLOVER: Okay so that was going to be my next question. So if everything looks good then you just go from there and if something happens like later then you just address that.
DOCTOR JAN PENVOSE-YI: And it’s a classic. I’m sure every mom out there has had the story whose done this [inaudible] movement a lot of them will say, now the baby’s moving. We put them on the monitor, we get beautiful, I always call the textbook perfect reactive strip and they always laugh and they’re oh I’m so sorry. I said, good now we know.
STEPHANIE GLOVER: Your car’s making a noise and you take it in and it stops making the noise
DOCTOR JAN PENVOSE-YI: Yeah. You’re going to get your haircut, it looks great that day
STEPHANIE GLOVER: And then if, so the test shows fetal distress, clearly you mentioned you’re going to be, you know, maybe rescheduling. Are there ever any instances where a rescheduled NST or maybe a bio profile isn’t enough? Do you ever have to be more reactive or?
DOCTOR JAN PENVOSE-YI: So basically it’s not necessarily the negative things that happen that the test is good for, it’s more of a good test if it looks reactive and it looks good
STEPHANIE GLOVER: Okay
DOCTOR JAN PENVOSE-YI: What do we do when it doesn’t is the question. So, there are some things that might just require a little bit more monitoring. Not totally distressful but we don’t want to take you off the monitor just yet because of course the baby’s inside your belly, swimming around in there, grabbing the umbilical cord every so once in a while. And you might get the heart rate deceleration and it’s just an accident. And we don’t monitor moms all the time so of course we might have some negative things that we see that don’t really mean anything.
STEPHANIE GLOVER: Okay
DOCTOR JAN PENVOSE-YI: So what you’re looking for is a recurrent pattern of these “bad things”. So you’re going to further evaluate with the ultrasound to tell you what to do next and or just send them straight. If you don’t really like what it’s looking like but you feel like they’re safe enough for transport to the hospital, you’ll say okay time to drive her to the hospital, sit on this monitor a lot longer in a more comfortable bed.
STEPHANIE GLOVER: Okay, and then they would just be in like labor and delivery . . .
DOCTOR JAN PENVOSE-YI: Yeah and then evaluated. Sometimes we will repeat the biophysical profile technically not in, technically you’re not supposed to do that unless you have a certain period of time. But you know, sometimes the baby is just sleeping and just comes at the wrong time. You need to see it again.
STEPHANIE GLOVER: Okay. For the panelists, do you have any other additional experiences with the test that you’d want to share that you’d have to repeat them or did you get some comfort from them
AMY DUGAN: I actually had kind of what the doctor was talking about in the last scenario where I was forty plus six with my first and woke up one night, thought maybe my water had broken, it didn’t. But I went to labor and delivery just the same and you know got checked out and just, while I happen to be there. On the monitor they noticed consistent decelerations and so I actually ended up getting induced the following morning because of those decelerations. And then ultimately had a caesarean because my daughter was very tightly wrapped in her umbilical cord. So, you know
STEPHANIE GLOVER: She was having too much fun on it
AMY DUGAN: Yeah, you know it was actually kind of mother’s intuition that I just went in that night and you know all turned out to be,
STEPHANIE GLOVER: Which I hear a lot
AMY DUGAN: Yeah so definitely listen to your mother’s intuition. Don’t feel silly, don’t feel like your burdening the staff by going in to get checked and sometimes it’s for good reason.
DOCTOR JAN PENVOSE-YI: Yeah I agree with that, I agree with that.
STEPHANIE GLOVER: Definitely and like she said too, I mean, if nothing else then you have some reassurance too so kind of either way you’re in good hands with them.
SUNNY GAULT: There was a non-stress test that I had. I totally forgot about until you had mentioned that and that was when I was pregnant with the girls. At about twenty, twenty-one weeks, I started feeling mild contractions. And I got really concerned about it because I knew that twins weren’t viable at that point. And so, I think I called, I called over to the hospital and I kind of explain the situation. They said well just come in, we’ll monitor you for a little bit. See how things are going. And they did the same thing. You know they hook me up to the monitors and monitored, you know, look for things for a while and I was still having contractions but they were looking at the cervix. They were looking at a bunch of different things to see if I had more signs of this actually being in labor.
But I was scared to death. I thought okay, pushed it too far. And as it turned out they told me that I was just dehydrated. And I was bringing on some labor contractions. But that was, that was a thing kind of a mommy intuition. I was like, I do not feel comfortable with this, I don’t, I’m one of those people that I don’t really had much bricks and hicks or anything like that until it was go time. I really didn’t have any signs of labor.
So, when this happened, it was really scary. And so, that did bring a lot of peace of mind from that. And it was my wakeup call and I actually ended up taking much better care of myself because I was like, oh I don’t want to be in that position again
STEPHANIE GLOVER: Right. And because there can be simple factor, you know, some of the things that you can do to improve the results and improve the baby’s, you know, condition. But you don’t know that until you’re in there so
SUNNY GAULT: I know. I know yeah
STEPHANIE GLOVER: Well thank you so much Doctor Jan Penvose-Yi for joining us today. For information about the Doctor as well as information about any of our panelists, visit our episode page on our website. This conversation continues for members of our Preggie Pals club. After the show, Doctor Penvose-Yi is going to be discussing the difference between non-stress tests and bio-physical profiles. To join our club, you can visit our website at www.newmommymedia.com
[Theme Music]
ANNIE LAIRD: Hi Preggie Pals, we have a question for one of our experts. Joan in New York writes: I’m in my third trimester and I have these itchy reddish, purplish bumps all over my belly. It’s driving me nuts. What is this? How can I get some relief?
EXPERT: Hi Joan, my name is Ray Kamali I’m an OBGYN and practicing in San Diego. Third-trimester rash, itching can be caused by a number of ideologies. However, based on your description, you may have a condition called puppps. Puppps spells P-U-P-P-P-S and it’s the most common specific dermatological condition of pregnancy.
It complicates somewhere between one and one sixty to one and three hundred pregnancies. It is diagnosed clinically based on characteristic findings on history and physical examination. Puppps typically presents as red bumps within the stretch marks or abdominal folds. This condition can extend to the extremities but the face, palms and soles are usually spared.
There’s also fairly severe itching associated with this condition. Treatment is supportive to help improve symptoms and may include [inaudible] anti-histamine such as benadryl and [inaudible] steroids as initial therapy. Early delivery is rarely recommended as this condition does not an effect of fetus. There are number of other conditions that can threaten the health of the baby including [inaudible] so it’s important to consult your prenatal care provider for the accurate diagnosis
[Theme Music]
STEPHANIE GLOVER: That wraps up our show for today. We appreciate you listening to Preggie Pals.
Don’t forget to check out our sister shows
• Parent Savers for parents with new born, infants and toddlers
• Twin Talks for parents of multiples
• Our show The Boob Group for moms who breastfeed their babies
This Preggie Pals; “Your Pregnancy Your Way”
[Disclaimer]
This has been a New Mommy Media production. Information and material contained in this episode are presented for educational purposes only. Statements and opinions expressed in this episode are not necessarily those of New Mommy Media and should not be considered facts. Though information in which areas are related to be accurate, it is not intended to replace or substitute for professional, Medical or advisor care and should not be used for diagnosing or treating health care problem or disease or prescribing any medications. If you have questions or concerns regarding your physical or mental health or the health of your baby, please seek assistance from a qualified health care provider.
SUNNY GAULT: New Mommy Media is expanding our line up of shows for new and expecting parents. If you have an idea for a new series or if you’re a business or organization interested in joining our network of shows through a co-branded podcast, visit www.NewMommyMedia.com .
[00:28:20]
[End of Audio]